| front |1 |2 |3 |4 |5 |6 |7 |8 |9 |10 |11 |12 |13 |14 |15 |16 |17 |18 |19 |20 |21 |22 |23 |24 |review |
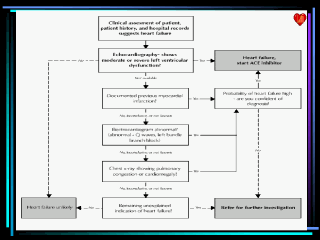 |
COMMON DIAGNOSTIC STUDIES Accurate diagnosis of heart failure is important. Electrocardiography. In most instances, left ventricular systolic dysfunction is caused by ischemic heart disease. Standard 12-lead electrocardiography should be used to determine whether ischemic heart disease is likely, so that appropriate interventions can be initiated. In addition, electrocardiography can provide information about rhythm abnormalities. Assessment of Ejection Fraction. The management of heart failure is based on the clinical presentation, the findings of the physical examination and the determination of systolic dysfunction by measurement of the left ventricular ejection fraction. Documentation of systolic dysfunction is critical to guide therapy. Transthoracic Echocardiography and Radionuclide Ventriculography. Transthoracic (standard surface) echocardiography is noninvasive and provides diagnostic information readily and safely. It gives information about ventricular function, chamber size and shape, wall thickness and valvular function. All such information is helpful in the management of patients with heart failure. Transthoracic echocardiography is inexpensive, reliable and widely available. Radionuclide ventriculography also may be used to assess left ventricular and right ventricular ejection fractions. Although this modality provides reproducible quantification of the ejection fraction, it does not yield information about valvular function or wall thickness. Echocardiography should be performed to guide management in patients with a presumed diagnosis of heart failure. The results can help to differentiate systolic from diastolic dysfunction and clarify relevant valvular dysfunction, as these disorders may be managed quite differently from systolic dysfunction. Exercise Stress Testing and Cardiac Catheterization. Exercise stress testing is useful for evaluating active and significant concomitant coronary artery disease, and it may have a role in assessing the degree of cardiac disability. Thus, it may be helpful in the evaluation of some patients with heart failure. The decision to perform exercise stress testing should be individualized. Blanket application in all patients is not indicated. Consultation with a cardiologist may be helpful in deciding when and exactly how to perform stress testing in appropriate patients. Cardiac catheterization is useful in the management of heart failure when the discovery of significant coronary artery disease or valvular heart disease would affect medical treatment or provide the necessary information to proceed to surgery. Coronary artery bypass grafting in multivessel disease with depressed systolic function decreases mortality and significantly improves symptoms of angina. The decision to proceed to cardiac catheterization should be determined by the clinical presentation, particular features in the patient, the results of noninvasive tests and a substantial weighing of the risks and benefits of the procedure. The decision to perform cardiac catheterization should be individualized and is best made in collaboration with a cardiologist. Ambulatory Rhythm Monitors. Sudden death, presumably because of arrhythmias, is a major cause of mortality in patients with heart failure. Over the past few years have shown that implantable cardioverter-defibrillators provide a major survival advantage in patients who have symptomatic or inducible ventricular arrhythmias and ischemic heart disease, with or without heart failure . Ambulatory monitoring should be performed when rhythm disturbance is suspected in a patient with heart failure. If a ventricular arrhythmia is present, the patient should be referred for further evaluation. 1. Pitt B, Zannad F, Remme WJ, Cody R, Castaigne A, Perez A, et al. The effect of spironolactone on morbidity and mortality in patients with severe heart failure. Randomized Aldactone Evaluation Study Investigators. N Engl J Med 1999;341:709-17. 2. Elefteriades JA, Tolis G Jr., Levi E, Mills LK, Zaret BL. Coronary artery bypass grafting in severe left ventricular dysfunction: excellent survival with improved ejection fraction and functional state. J Am Coll Cardiol 1993;22:1411-7. 3. Moss AJ, Hall WJ, Cannom DS, Daubert JP, Higgins SL, Klein H, et al. Improved survival with an implanted defibrillator in patients with coronary disease at high risk for ventricular arrhythmia. Multicenter Automatic Defibrillator Implantation Trial Investigators. N Engl J Med 1996;335:1933-40. |